
By Dr Ankita Jain
Consultant Obstetrician & Gynaecologist
March 24, 2026
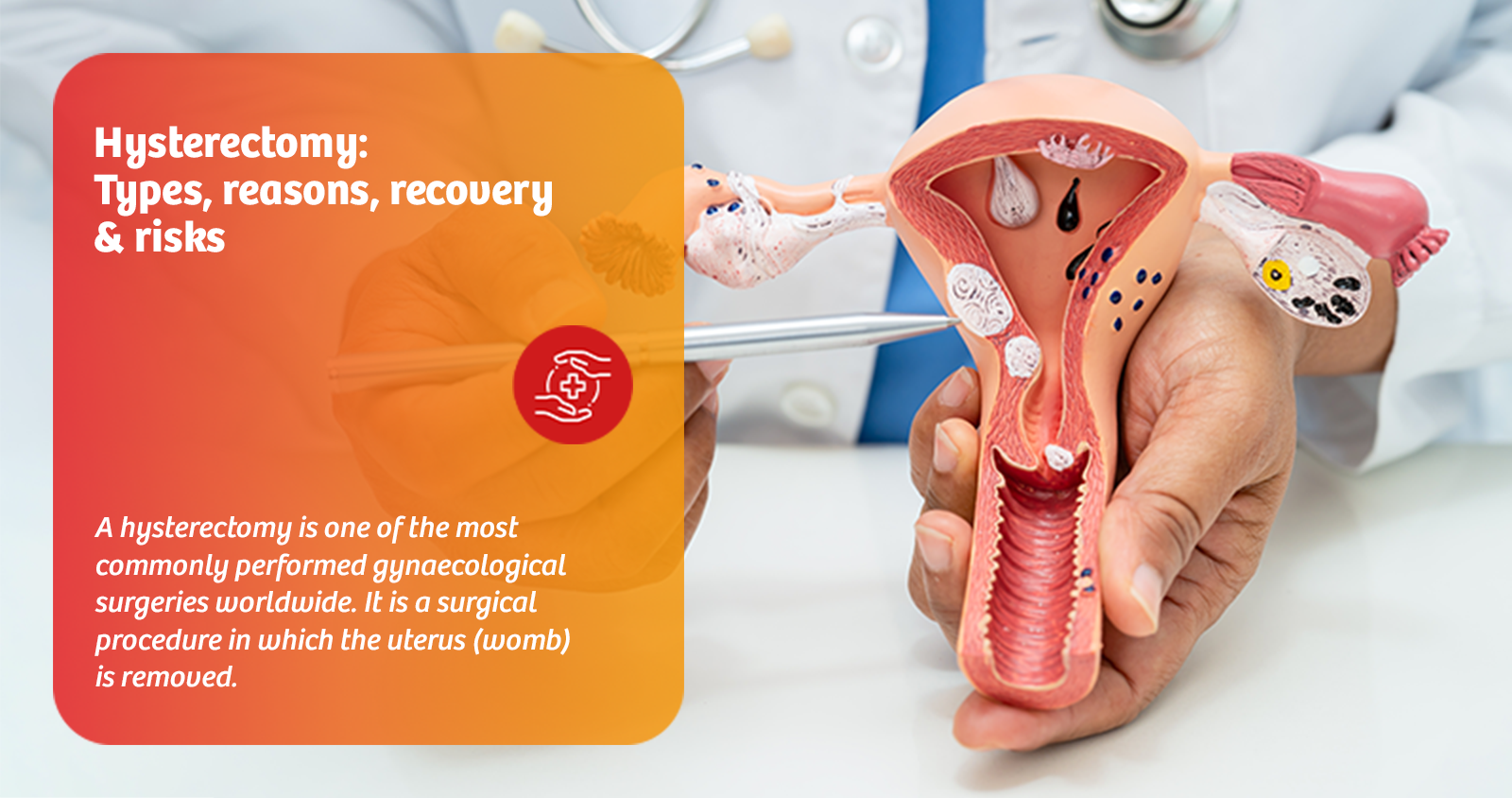
A hysterectomy is one of the most commonly performed gynaecological surgeries worldwide. It is a surgical procedure in which the uterus (womb) is removed. Depending on the reason for surgery and the patient's condition, the ovaries, fallopian tubes, and cervix may also be removed.
After a hysterectomy, a woman can no longer become pregnant and will no longer have menstrual periods.
Gynaecologists recommend a hysterectomy when other treatments have failed or when the condition is severe. The most common indications for hysterectomy include
1. Uterine fibroids
Uterine fibroids are non-cancerous growths in or on the uterus. They can cause heavy bleeding, pelvic pressure, and pain. When fibroids are large or multiple and conservative management fails, a hysterectomy is often the definitive solution.
2. Endometriosis
Endometriosis occurs when tissue similar to the uterine lining grows outside the uterus. Severe cases that do not respond to hormonal therapy or laparoscopy may require hysterectomy.
3. Uterine prolapse
When the uterus slips down into or protrudes out of the vagina due to weakened pelvic floor muscles, a hysterectomy can provide permanent relief.
4. Abnormal uterine bleeding (AUB)
Heavy or irregular menstrual bleeding that does not respond to medication or other procedures may necessitate hysterectomy.
5. Gynaecological cancers
Cancers of the uterus (endometrial cancer), cervix, or ovaries often require hysterectomy as part of cancer treatment.
6. Adenomyosis
When the inner lining of the uterus grows into the muscular wall (myometrium), causing painful, heavy periods, hysterectomy may be recommended.
7. Chronic pelvic pain
Unmanageable pelvic pain due to uterine pathology may be treated with a hysterectomy when all other options are exhausted.
Understanding the types of hysterectomy helps patients make informed decisions with their gynaecologist.
1. Total hysterectomy
The uterus and cervix are completely removed. This is the most common type performed.
2. Partial (Subtotal or supracervical) hysterectomy
Only the upper part of the uterus is removed; the cervix is left in place. This option preserves cervical function but still requires Pap Smear screening.
3. Radical hysterectomy
The uterus, cervix, upper part of the vagina, and surrounding tissues are removed. This is typically performed for gynaecologic cancers.
4. Hysterectomy with oophorectomy
Modern gynaecological surgery offers multiple approaches. Your surgeon will recommend the most appropriate method based on the size of your uterus, the reason for surgery, and your overall health.
1. Abdominal hysterectomy
The uterus is removed through a horizontal or vertical incision in the lower abdomen. This approach provides the surgeon with a wide field of view and is used for large uteruses or complex cases. Recovery time is longer (6–8 weeks).
2. Vaginal hysterectomy
The uterus is removed through the vagina without any abdominal incisions. It has fewer complications, shorter hospital stays, and faster recovery (3–4 weeks). Ideal for uterine prolapse.
3. Laparoscopic hysterectomy
Small incisions are made in the abdomen, and a laparoscope (tiny camera) guides the surgery. Less invasive with faster recovery (2–3 weeks).
4. Robot-assisted laparoscopic hysterectomy
Similar to laparoscopic, but uses robotic arms controlled by the surgeon for enhanced precision. Suitable for complex cases.
Before surgery, your gynaecologist will
Patients are usually advised not to eat or drink after midnight before surgery.
Recovery time varies by surgical approach
| Approach | Hospital stay | Full recovery |
| Abdominal | 3–5 days | 6–8 weeks |
| Vaginal | 1–2 days | 3–4 weeks |
| Laparoscopic | 1–2 days | 2–3 weeks |
| Robotic | 1–2 days | 2–3 weeks |
Like all major surgeries, a hysterectomy carries potential risks:
Discuss all risks thoroughly with your surgeon before consenting to the procedure.
Will I go through menopause?
Can I still have sex?
Yes. Most women resume sexual activity after 6–8 weeks. Many report improved sexual satisfaction due to relief from chronic pain or heavy bleeding.
Emotional impact
Some women feel relief after surgery; others may grieve the loss of reproductive ability. Counselling and support groups are valuable resources.
Long-term considerations
Before opting for a hysterectomy, consider less invasive alternatives
Always discuss all options with a qualified gynaecologist before surgery.
Consult your gynaecologist immediately if you experience
Q: Is a hysterectomy a major surgery?
Yes, it is a major gynaecological surgery requiring anaesthesia, hospitalisation, and a recovery period of 2–8 weeks.
Q: Will I gain weight after a hysterectomy?
Weight gain is not a direct consequence, but hormonal changes (if ovaries are removed) can affect metabolism. A healthy diet and exercise help manage weight.
Q: Can fibroids come back after a hysterectomy?
No. Since the uterus is removed, uterine fibroids cannot recur.
Q: Is a hysterectomy safe for older women?
Yes, but surgical risk increases with age and pre-existing conditions. A thorough pre-operative evaluation is essential.
Q: How long does a hysterectomy operation take?
Typically 1–3 hours, depending on the type and surgical approach.
Best gynaecological care in Ahmedabad.
A hysterectomy is a life-changing but often necessary gynaecological procedure that can significantly improve quality of life when performed for the right indications. Modern surgical techniques have made hysterectomy safer, with shorter recovery times and fewer complications than ever before.
If you or a loved one has been advised to undergo a hysterectomy, it is important to have an open and detailed discussion with your gynaecologist—covering your symptoms, all available treatment options, and what to expect before, during, and after the surgery.